Emma Reed
March 13, 2026
Stress Headaches vs. Migraine: How to Spot Patterns Safely and Plan Better Days
If you get recurring head pain, one of the most confusing questions is simple: what kind of headache is this, and why today?
Many people use broad labels like “stress headache” or “migraine day” based on how bad they feel in the moment. That is understandable, but it can blur useful details. Two difficult headache days can feel equally miserable while having very different patterns, triggers, and recovery timelines.
This guide is educational and non-diagnostic. It does not provide diagnosis, treatment plans, or cure claims. The goal is practical: help you build a safer way to observe patterns so daily decisions become easier and clinical conversations become clearer.
Why “just memory” usually fails
When symptoms are disruptive, memory tends to keep the dramatic parts and lose context. You may remember the worst pain, but forget that sleep was short for three days, lunch was delayed, or your screen time doubled.
Without structure, common thinking errors appear:
- Recency bias: today’s event feels like the whole trend.
- Single-cause bias: we pick one trigger and ignore stacked factors.
- Relief bias: if pain improves after one change, we assume that change caused improvement.
A headache log does not remove uncertainty. It reduces avoidable confusion.
A practical distinction: stress-type pattern vs migraine-like pattern
Only a licensed clinician can diagnose. But pattern awareness still helps daily planning.
Stress-type pattern (often described by users as “tension” days)
People commonly report:
- Dull, pressing, or tight sensation
- Band-like discomfort around forehead, temples, or back of head
- Mild to moderate intensity
- Function possible but unpleasant
- Often linked to posture strain, jaw clenching, long focus blocks, poor breaks, dehydration, or emotional stress
Migraine-like pattern
People commonly report:
- Moderate to severe intensity, sometimes throbbing
- Worse with routine activity
- Nausea and/or sensitivity to light, sound, or smell
- Need to reduce activity or rest in a darker, quieter environment
- May include warning changes before pain (fatigue, mood change, food craving, neck discomfort, visual disturbances in some people)
Real life is messy. Mixed features are common. That is exactly why logging details beats guessing labels.
The 5-layer tracking model that actually works
Most logs fail because they are either too shallow (“headache: yes/no”) or too heavy (so many fields that nobody keeps it up). A sustainable model has five layers:
- Episode basics (start time, end time, intensity trend)
- Symptoms (pain location/quality + associated symptoms)
- Context (sleep, meals, hydration, stress, screen load, activity)
- Actions taken (rest, hydration, break, medication if any, timing)
- Outcome (time to meaningful relief, recurrence within 24 hours, function impact)
If you fill these reliably, your data quality improves within two weeks.
What to log during each episode
Use short, objective language first. Interpret later.
Episode template
- Start: 14:10
- Peak intensity: 7/10 at 15:00
- Location: right temple + around eye
- Quality: throbbing, pressure in neck
- Associated signs: light sensitivity, mild nausea
- Activity impact: stopped deep work for 90 minutes
- Actions: water, snack, 20-minute dark-room rest, medication at 15:15 (if used)
- Relief: down to 3/10 by 17:00
- Recurrence: returned to 5/10 at 21:30
Notice what this avoids: no confident claims like “caused by weather.” It records facts you can test later.
Daily context checklist (2 minutes)
Most pattern signals come from ordinary routines. Track these once per day even if no episode occurs.
- Sleep duration and sleep quality (same scale each day)
- First meal timing and long gaps between meals
- Approximate hydration rhythm
- Caffeine timing/amount changes
- Stress load (low/medium/high)
- Screen intensity (normal/high/very high)
- Physical tension markers (jaw clenching, shoulder tightness, neck stiffness)
- Menstrual cycle phase if relevant
- New supplements, illnesses, travel, unusual schedule changes
No precision theater needed. Consistent rough data is more useful than perfect data for three days followed by nothing.
Confounders: the hidden reason patterns look random
A confounder is a factor that can mimic, amplify, or hide another factor. Headache patterns are full of them.
Common confounder clusters:
- Sleep debt + stress spike
- Skipped meal + high caffeine + intense meetings
- Long gaming/work session + poor posture + low hydration
- Travel disruption + irregular meals + poor sleep environment
When people say “my headaches are random,” they often mean “my confounders are untracked.”
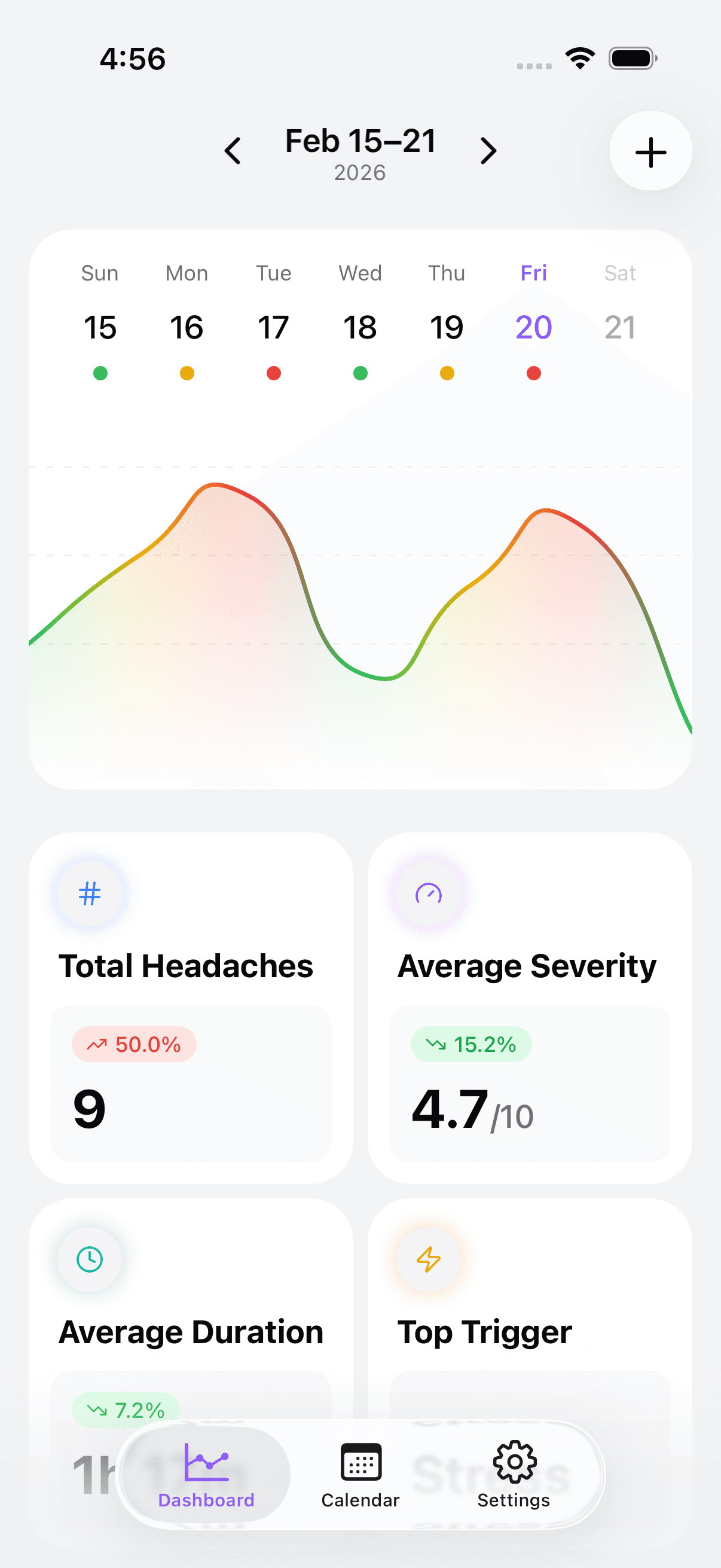
Example: turning noise into a pattern
Suppose you log 21 days and find 9 headache episodes. At first glance, weather seems suspicious. But review shows:
- 7/9 episodes happened on days with sleep <6.5 hours
- 6/9 followed a meal gap >6 hours
- 5/9 occurred after two or more back-to-back high-focus screen blocks
- Weather shifts happened too, but on many non-headache days as well
Takeaway: weather may contribute, but routine strain appears more actionable.
That gives practical next steps without pretending certainty.
Weekly review script (10–15 minutes)
Use this exact review flow once per week:
- Count episodes and compare to prior week.
- Mark top associated factors (not “causes,” just associations).
- Check timing patterns (morning, afternoon, evening).
- Review function impact (work blocks missed, social plans changed, sleep disrupted).
- Choose one adjustment for next week.
Good adjustment examples:
- Add a planned snack window on high-focus days.
- Insert a 5-minute movement break every 60–90 minutes.
- Move caffeine earlier and reduce late-day intake.
- Build a wind-down buffer before sleep.
Do one change at a time when possible. Multiple simultaneous changes make interpretation harder.
Monthly summary format for clinician visits
Bring one page, not a chaotic notebook. Include:
- Episode count per week
- Typical intensity range
- Most frequent associated symptoms
- Most common context factors
- What you tried and what seemed to help/not help
- Questions you want answered
This saves appointment time and makes your report more clinically useful.
Suggested neutral question style:
- “I noticed episodes cluster with short sleep and long meal gaps. What should I monitor next?”
- “These symptoms recur together. Which warning signs mean I should seek urgent care?”
- “How can I track response to our plan in a way that is most useful for follow-up?”
Red flags: when to seek urgent medical care
Tracking is not a replacement for emergency evaluation. Seek urgent professional care for severe or concerning symptoms, such as:
- Sudden, unusually severe headache
- Headache with chest pain, breathing difficulty, fainting, confusion, seizure, or major neurologic change
- New severe headache after head injury
- Persistent vomiting or inability to keep fluids down
- High fever with severe head pain and neck stiffness
- Any rapidly worsening pattern that feels alarming or clearly different from usual
If unsure, prioritize safety and contact local medical services.
Common mistakes that reduce data quality
- Changing scales every few days
- Backfilling many days from memory
- Logging only painful days (misses comparison data)
- Labeling causes too early
- Ignoring medication timing and recurrence
- Overcomplicating the form until you stop using it
Your best system is the one you can keep for months.
A realistic 14-day starter plan
If your current tracking habit is inconsistent, use this reset:
Days 1–3
- Log only episode basics and one daily context note.
Days 4–7
- Add symptom details and action timing.
Days 8–14
- Add sleep/meal/screen/stress checkboxes daily.
- Do your first weekly review on day 14.
Goal: consistency before complexity.
Gentle language, better decisions
You do not need to prove a single trigger to make progress. You need enough reliable observations to make safer next decisions.
A useful mindset:
- Replace “X caused this” with “X often appears before this.”
- Replace “nothing works” with “relief was faster on days I did A early.”
- Replace “it is random” with “I need two more weeks of clean logs.”
This is less dramatic, more accurate, and usually more helpful.
Final takeaway
If headache days are affecting your quality of life, a structured log can reduce uncertainty and improve planning. Keep entries short, objective, and consistent. Review weekly. Escalate safety concerns quickly. Bring clear summaries to licensed clinicians.
You are not trying to become your own specialist. You are building better information so the right decisions become easier.
Educational note: This article is informational only and not medical advice. It does not provide diagnosis, individualized treatment, or cure claims.