Emma Reed
March 24, 2026
Transition-Day Headaches: A Practical Plan for Smoother Mondays, Return-to-Work Days, and Schedule Swaps
If your headaches seem to show up on Mondays, after travel days, after night shifts, or right when your routine changes, you are not imagining it. Many people notice that headache patterns are less about a single trigger and more about abrupt transitions: sleep timing shifts, delayed meals, extra caffeine, long screen blocks, dehydration, and stress hormones changing all at once.
The good news is that you do not need a perfect lifestyle to reduce transition-day headache risk. You need a repeatable system that makes schedule changes less abrupt. This guide gives you a practical, medically cautious framework you can test over four weeks using your headache tracker.
Important note: this article is educational, not a diagnosis or a cure plan. Headaches can have many causes. If headaches are severe, new, rapidly worsening, or include neurologic symptoms, seek urgent medical care.
Why transition days are common headache days
A transition day is any day when your internal rhythm and your external schedule stop matching. Common examples:
- Weekend to weekday shift
- Vacation back to work
- Day shift to evening or night shift
- Travel day across time zones
- Big deadline day after lighter days
On these days, several headache-related stressors can stack:
- Sleep timing moves suddenly (bedtime/wake time shifts)
- Hydration pattern changes (coffee replaces water)
- Meal timing drifts (long gaps without food)
- Caffeine timing changes (too late, too much, or too little)
- Screen exposure jumps (meetings, email, admin catch-up)
- Muscle tension increases (neck, jaw, upper back)
- Stress ramps early (anticipation and time pressure)
Any one of these may be manageable. Several together can push you over your threshold.
The threshold model: useful, simple, and actionable
Think of headache risk as a bucket. Every stressor adds water to the bucket. A headache is more likely when the bucket overflows. This model is not perfect science for every person, but it is practical.
Your job is not to eliminate every trigger. Your job is to lower the total load on transition days.
That means:
- Keep sleep and wake times closer together across days
- Protect hydration and meals early in the day
- Keep caffeine steady, not chaotic
- Insert short recovery breaks before symptoms escalate
- Use tracking data to adjust one variable at a time
A 24-hour transition-day protocol
Use this protocol the evening before and the day of your transition.
Evening before (10-20 minutes)
- Confirm wake time for tomorrow
- Set out a water bottle where you will see it
- Decide first meal time (or first snack if mornings are hard)
- Decide caffeine window (for example, first dose within 90 minutes of waking, last dose by early afternoon)
- Pick one short movement break you can actually do (5-10 minutes)
This is intentionally small. Decision fatigue is real. Pre-deciding removes friction.
First 2 hours after waking
- Drink water soon after waking
- Eat something with protein + carbohydrate
- Keep caffeine amount close to your usual baseline
- Get daylight if possible, even briefly
- Avoid immediate marathon screen sessions if you can
You are telling your nervous system: today is predictable.
Midday stabilization
- Avoid long fasting gaps
- Refill water intentionally, not only when thirsty
- Add a short neck/shoulder mobility break
- If you use analgesics, avoid reactive overuse patterns and follow label/clinician advice
Late afternoon protection
- Keep caffeine late-day intake low or none
- Lower visual load in the last work block if possible
- Reduce unnecessary decision load (batch small tasks)
Evening wind-down
- Keep bedtime near target, even if the day felt messy
- Limit doom-scrolling if sleep is already fragile
- Note headache intensity and possible contributors in your tracker
Consistency beats perfection.
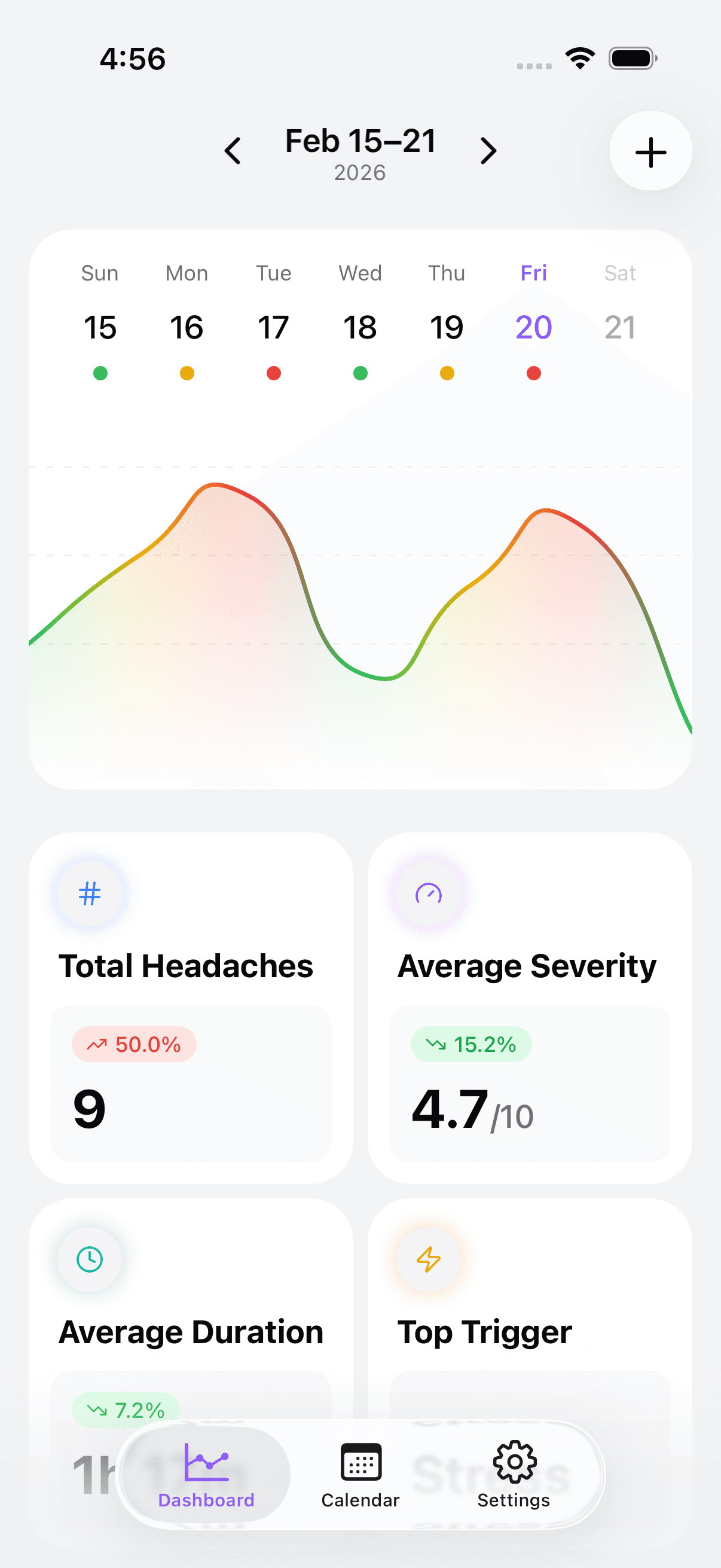
Build your personal “transition profile” in a headache tracker
Generic advice helps only so much. Your tracker turns guesses into patterns.
Track these fields consistently on transition days:
- Sleep start/end times
- Sleep quality rating
- First hydration time
- Caffeine amount and timing
- Meal timing (especially first and longest gap)
- Screen hours before first symptom
- Stress level (morning, midday, evening)
- Neck/jaw tension rating
- Headache onset time and intensity
- Medication use (type, dose, time)
After 3-4 weeks, look for repeat patterns instead of single events.
Examples:
- Headaches mostly appear when first meal is delayed past noon
- Headaches rise when caffeine is both increased and taken later
- Headaches cluster after nights with less than your usual sleep window
- Headaches are milder when you took two movement breaks before noon
These are actionable patterns.
Four-week experiment plan (low friction)
Do not change everything at once. Use small experiments.
Week 1: Baseline only
Track without trying to optimize. Learn your current pattern.
Goal: data quality, not behavior change.
Week 2: Hydration + first meal timing
Pick two anchors:
- Water within the first hour of waking
- First meal/snack within a fixed window
Keep all else mostly unchanged.
Week 3: Caffeine timing consistency
Hold total caffeine near baseline and tighten timing.
Examples:
- Same first-cup window each day
- No caffeine after a specific time
Week 4: Screen and tension breaks
Add two brief breaks before symptom-prone periods.
Ideas:
- 2 minutes eye rest every 30-45 minutes of continuous screen work
- 5 minutes neck/shoulder movement late morning
- Jaw unclenching check-ins during stressful tasks
At the end of week 4, compare transition-day headache frequency and average intensity to week 1.
What to do when a headache starts anyway
Even with good planning, headaches can still happen. A response plan can prevent escalation.
- Pause and assess early: where are you on intensity 0-10?
- Hydrate and fuel if you likely under-ate or under-hydrated
- Reduce input load: lower brightness, reduce noise, step away briefly
- Release tension: jaw, neck, shoulders, and posture reset
- Use your usual treatment plan safely (per label or clinician guidance)
- Log what helped within the next few hours
Early action is often more useful than waiting until pain is severe.
Medication safety and overuse awareness
Frequent rescue-medication use can itself become part of a headache cycle for some people. This is often discussed as medication-overuse headache risk.
Practical safety reminders:
- Follow package instructions and clinician advice
- Avoid combining products with overlapping ingredients unintentionally
- Track how many days per month you use acute medications
- If usage is climbing, discuss with a healthcare professional early
Your tracker is valuable here because memory is imperfect under stress.
Red flags: when to seek urgent care
Get urgent medical evaluation for headache with any of the following:
- “Worst headache of your life” or thunderclap onset
- New neurologic symptoms (weakness, confusion, speech or vision changes)
- Fever, stiff neck, or severe systemic illness signs
- Headache after head injury
- New headache pattern during pregnancy or postpartum
- New persistent headache after age 50
If something feels wrong, trust that signal and seek care.
Transition scenarios and micro-adjustments
1) Monday headaches after weekend schedule drift
Try:
- Keep weekend wake time within about 60-90 minutes of weekday target
- Shift Sunday bedtime gradually earlier
- Front-load hydration and breakfast Monday morning
2) Return-from-travel headaches
Try:
- Re-establish local wake/light exposure quickly
- Keep caffeine close to destination morning
- Hydrate deliberately during and after travel
- Schedule a lighter first work block if possible
3) Shift-change headaches
Try:
- Use a fixed pre-shift routine (meal, hydration, brief movement)
- Protect a dark, quiet sleep window between shifts
- Keep caffeine targeted to early shift window
4) Post-deadline crash headaches
Try:
- Add mini-recovery blocks the day after high-stress pushes
- Normalize meals and hydration before catching up on low-priority tasks
- Reduce unnecessary screens when possible
The theme is the same: reduce abrupt swings.
Sample transition-day checklist
Keep this short and repeatable:
- Water within 60 minutes of waking
- First meal/snack within planned window
- Caffeine amount and timing near baseline
- Two brief movement/tension breaks before noon
- No long fasting gap
- Late-day caffeine limit respected
- Headache metrics logged (onset, intensity, context)
If you miss two items, do not abandon the day. Resume the next item.
Common mistakes that make transition headaches worse
- Over-correcting with extreme caffeine swings
- Skipping meals to “catch up” on work
- Ignoring mild early symptoms until severe
- Changing too many variables at once (noisy data)
- Tracking inconsistently, then expecting clear patterns
Simple and consistent usually wins.
How to review your data monthly
Once per month, run a short review in your tracker:
- Count transition days
- Count headache days on transition vs non-transition days
- Compare average intensity
- Identify top two recurring contributors
- Pick one adjustment for next month
Examples of one-change plans:
- “I will keep first meal before 10:30 on transition days.”
- “I will keep caffeine start within a 60-minute window.”
- “I will schedule two movement breaks before first long meeting block.”
Small plans are easier to execute and evaluate.
The realistic goal
The goal is not zero headaches forever. The realistic goal is fewer high-disruption days, lower peak intensity, and faster recovery when headaches happen.
If your data shows partial improvement, that still matters. Reduced unpredictability improves work quality, mood, and confidence.
And if your pattern remains severe or hard to control, that is useful information to bring to a clinician. A well-kept tracker can make consultations more precise and efficient.
Bottom line
Transition-day headaches are often a stacking problem, not a personal failure. When schedule changes are unavoidable, a consistent protocol can reduce abrupt stress on your system.
Start with one transition checklist, track consistently for four weeks, and adjust with real data. No miracle claims, just practical risk reduction.
That is usually enough to make difficult days more manageable.